Background
The introduction of antibiotics revolutionised healthcare. However, over time, microbes developed resistance to them. This has meant that previously treatable diseases now pose a serious threat to public health, and to food security, sustainable development, animal husbandry, veterinary medicine, and research. Antibiotic resistance is a growing problem worldwide. Despite this, it is under-discussed and goes relatively unnoticed by most in society, causing it to be termed a ‘silent pandemic’.
Multiple factors are important in limiting the spread and impact of antibiotic resistance. For example, monitoring is essential to understand the spread, and more research is needed to determine how resistance develops, so that it can be prevented in future. In Sweden, a national liason was established by the government in 2012 to work on the topic of antibiotic resistance (Strama). The collaboration (2021-2025) is a continuation of a previous effort, and is focused on One Health, and is cross-sectorial. You can read more about this effort in publications, such as the guidelines for antibiotic resistance 2021-2025, from the Swedish Public Health Agency. The annual Swedres-Svarm report, co-produced by the Public Health Agency of Sweden (FoHM) and the National Veterinary Institute (SVA), evaluates statistics related to the sale of, and the development of resistance to, antibiotics for both humans and animals.
Novel antibiotics will be needed to treat currently antibiotic-resistant infections. However, the development of novel drugs and effective diagnostic tools is both time consuming and expensive. It is therefore important that this work starts as early as possible. Further, it is essential that policies are put in place to reduce the risk of microbes developing resistance to any new drugs.
Data highlights (2)
Editorials (2)
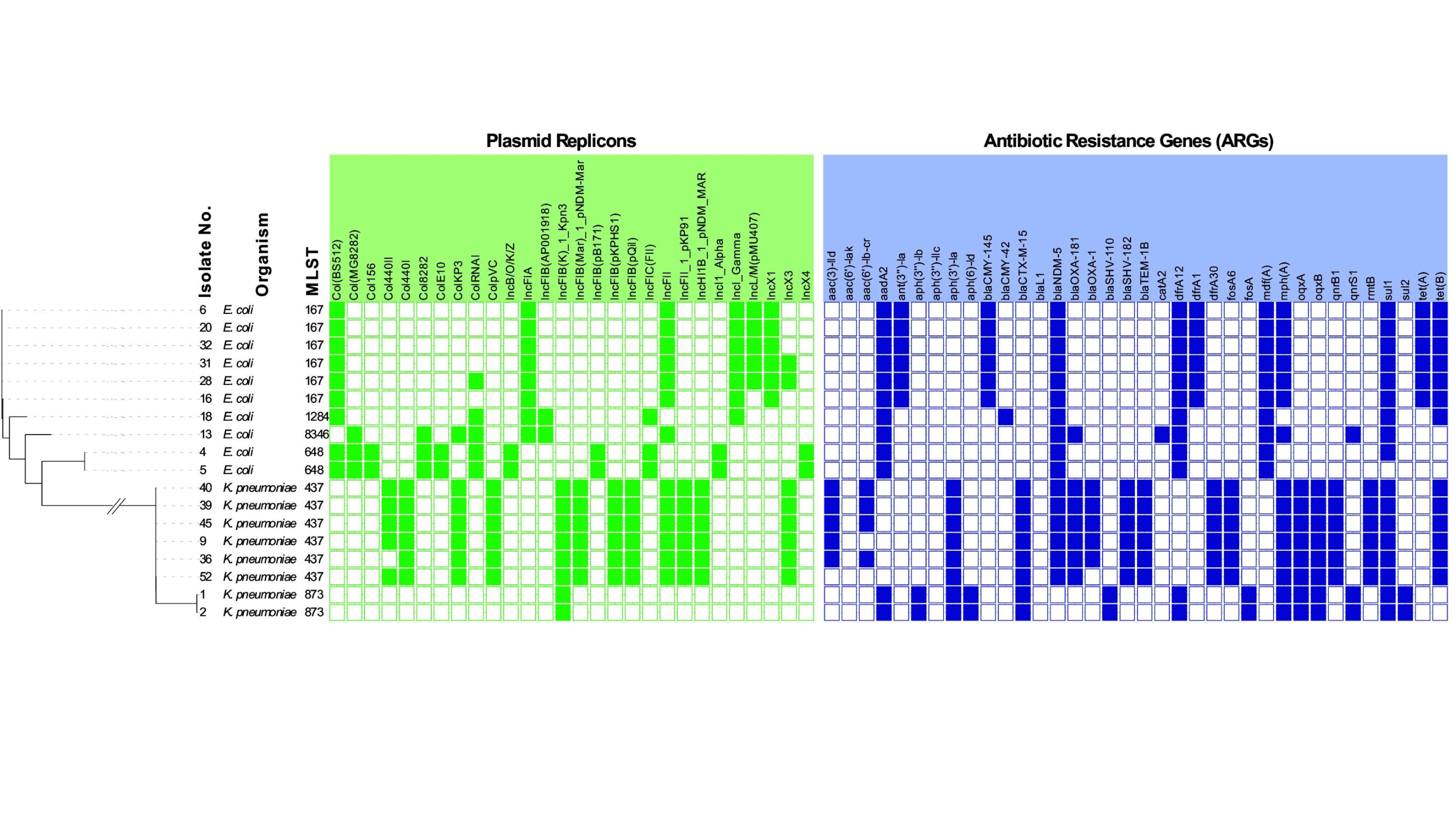
Antibiotic Resistance
Infectious Diseases Antibiotic Resistance
Ongoing research projects (12)
| Project title | Funder |
|---|---|
Bacterial Injection Machines within the Human Gut: Structure, Function and Potential as Novel Avenue in Precision Medicine to Battle Antimicrobial ResistanceHost institute:
Lund University |
Swedish Research Council |
Curing Sepsis - a personalized bench-to bedside approach for prediction and treatment of short and long-term complication in sepsisHost institute:
Lund University |
Swedish Research Council |
Epidermal Bioelectronics for Infection Monitoring in Human Skin WoundHost institute:
Karolinska Institute |
Swedish Research Council |